 Our fistula project previously operated in partnership with Fistula Free Nepal, however for a number of reasons, it has been operating as part of MeRO since February 2019.
Our fistula project previously operated in partnership with Fistula Free Nepal, however for a number of reasons, it has been operating as part of MeRO since February 2019.
MeRO accepts referrals for women with fistula who need surgical intervention for obstetric fistula and/or have conditions which may or may not be related to this obstetric injury. These range from cataracts to kidney stones, and like all patients at the Shelter, obstetric fistula affects women who usually live in remote regions and cannot afford medical care due to poverty. 
It is estimated there are 5000 women in Nepal who currently live with this preventable childbirth injury. Every year another 500 women develop this terrible condition which leaves them with permanent urinary and/or faecal incontinence depending on the location of the and severity of the fistula.
Initial fistula surgery in Nepal may be funded by a large American organisation that covers the cost of surgery in one of four different hospitals. Some women, however, are unable to access this and there are other expenses incurred during hospitalization that may not be included.
For all fistula affected women who present to the Shelter, everything is free.
What is a fistula?
Unless you are a doctor, nurse or a midwife, you probably have no idea what a fistula is because they are virtually unheard of in the developed world due to improved obstetric care and early intervention. If you would like to know a bit about fistulas we invite you to read on:
 A fistula is a tract that develops between one part of the body and another. Occasionally fistulas result from trauma caused by rape but approximately 97% of fistulas are obstetric fistulas – a preventable childbirth injury caused by prolonged obstructed labor. Fistulas are a huge problem because the majority of women who go on and develop an obstetric fistula have not only given birth to a stillborn baby, but have to contend with urinary and/or faecal incontinence.
A fistula is a tract that develops between one part of the body and another. Occasionally fistulas result from trauma caused by rape but approximately 97% of fistulas are obstetric fistulas – a preventable childbirth injury caused by prolonged obstructed labor. Fistulas are a huge problem because the majority of women who go on and develop an obstetric fistula have not only given birth to a stillborn baby, but have to contend with urinary and/or faecal incontinence.
During obstructed labour, continued contractions push the baby’s head against the mother’s pelvic bones exerting pressure which squishes the soft tissues between the baby’s head and the bones of the pelvis. Prolonged pressure reduces the blood flow and therefore the delivery of oxygen to these vital parts of the body causing tissue death. The dead tissue disintegrates and a tract or passage develops between the woman’s birth canal and bladder and/or rectum resulting in urinary and faecal incontinence.
Surely modern medicine can fix this?
Once a fistula has developed there is only one cure – surgery – but not all fistulas can be repaired. Fistula surgery is difficult and requires a correct diagnosis, highly qualified staff, access to specialized facilities, money (medical care is not free in Nepal) and individualized patient care. The surgical success rate is around 70 – 80%. For the remaining 20 – 30% life is desperate.
Why do fistulas develop?
There are many reasons why women in developing countries experience fistulas, however the main reasons are:
- Malnutrition caused by poverty and early marriage which prevents a woman’s pelvis from growing to the size that can easily deliver a baby
- Early marriage – Women who are married young and bear children at an early age are at risk because the pelvis is not fully developed. Obstructed labor is more likely to occur simply because the pelvis is not big enough, and with obstructed labor comes the risk of fistula formation. It is not uncommon for women to experience obstructed labor that can continue for several days before help is sought.
- Lack of access to both adequate antenatal assessment and
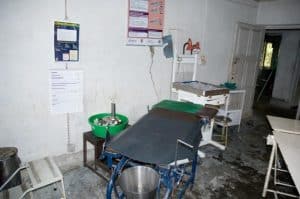 medical facilities – Only 33% of births throughout Nepal occur in health care facilities and 81% of Nepalese live in rural or remote poorly resourced regions. Early intervention, forceps deliveries and Caesarian sections are often simply not an option and many hospitals in Nepal do not even have operating theatres. This photo is of the maternity ward in a hospital in a remote region of Nepal.
medical facilities – Only 33% of births throughout Nepal occur in health care facilities and 81% of Nepalese live in rural or remote poorly resourced regions. Early intervention, forceps deliveries and Caesarian sections are often simply not an option and many hospitals in Nepal do not even have operating theatres. This photo is of the maternity ward in a hospital in a remote region of Nepal. - Lack of access to educated and skilled staff. It is difficult for fistula affected women to secure a correct diagnosis because public and professional knowledge of fistula is poor and even if these women are referred on, medical staff often simply do not have the specialized skills to treat them.
- Lack of access to transportation to access medical intervention due to poor infrastructure that comes with living in a remote region.
- Poverty – medical care is not free in Nepal so surgical intervention is often simply not affordable without external funding.
What are the consequences of fistula?
Fistulas have enormous physical, psychological, social and financial consequences for women who experience them. Left untreated, obstetric fistula results in a range of physical problems including frequent infections, kidney disease, painful sores and infertility. Physical consequences of fistulas result in psychological harm, distress and depression and physical and psychological consequences result in social and financial ones.
 Many women in Nepal with fistulas become marginalised and experience social isolation like this woman who lived in a cave. They are unable to work resulting in deepening poverty. They are shamed and abandoned by their husbands and families, and ostracized by their communities, driving them even further into poverty. It is estimated that approximately 30% of fistula affected women are abandoned so many women lose their husbands, loved ones, marriages, relationships, are sometimes forced to sleep away from family areas and have been found in shocking conditions.
Many women in Nepal with fistulas become marginalised and experience social isolation like this woman who lived in a cave. They are unable to work resulting in deepening poverty. They are shamed and abandoned by their husbands and families, and ostracized by their communities, driving them even further into poverty. It is estimated that approximately 30% of fistula affected women are abandoned so many women lose their husbands, loved ones, marriages, relationships, are sometimes forced to sleep away from family areas and have been found in shocking conditions.
How we help: We have a separate fund to help these women to ensure that they receive all medical and surgical intervention, nursing care and physiotherapy, and as with all of MeRO’s patients, everything is free.
